At Hunter Medical Research Institute, we’re delivering groundbreaking health and medical research that transforms the health and wellbeing of our communities.
At Hunter Medical Research Institute, we’re delivering groundbreaking health and medical research that not only transforms the health and wellbeing of communities in our region, but also right around the world.
We are Australia’s largest regional medical research institute, driving solutions across a diverse range of health areas that impact our communities.
From day one, we’ve been here for our community, just as they’ve been here for us. Our Institute tackles the biggest health challenges faced by the one million people in our Hunter New England region.
Our vision is not just a local or a regional one. We aim to discover local and cure global, making health discoveries in our region that are scalable and can be applied to transform health outcomes right around the world.
With more than 1700 researchers, staff and students in our ecosystem, our world-leading experts collaborate across multidisciplinary teams with one goal: to help our community be healthier and live their best lives.
RESEARCHERS, STAFF AND STUDENTS
COMMUNITY MEMBERS
RESEARCH PROGRAMS
At HMRI, we push our research further to make it relevant to everyday life.
We’re working in the lab and beyond. We’re thinking long term. We’re always listening and learning from our community to help us shape our research priorities, so we can make sure we’re providing impact where it’s needed most.
Every day, we’re taking healthy further.
We drive research that anticipates emerging health trends, issues, and challenges impacting the people in our communities.
We bring the brightest minds together to solve our region’s biggest health problems.
We house a comprehensive suite of services designed to accelerate research and research translation.


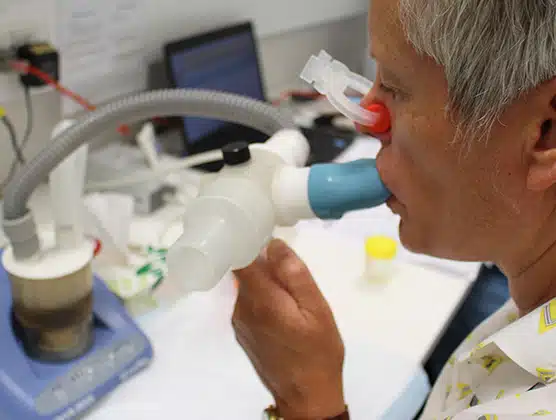
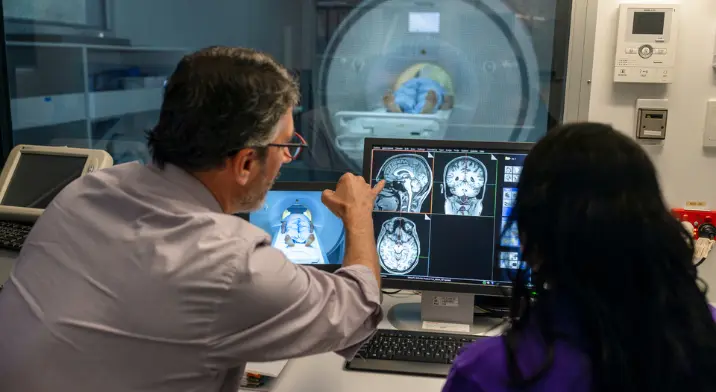






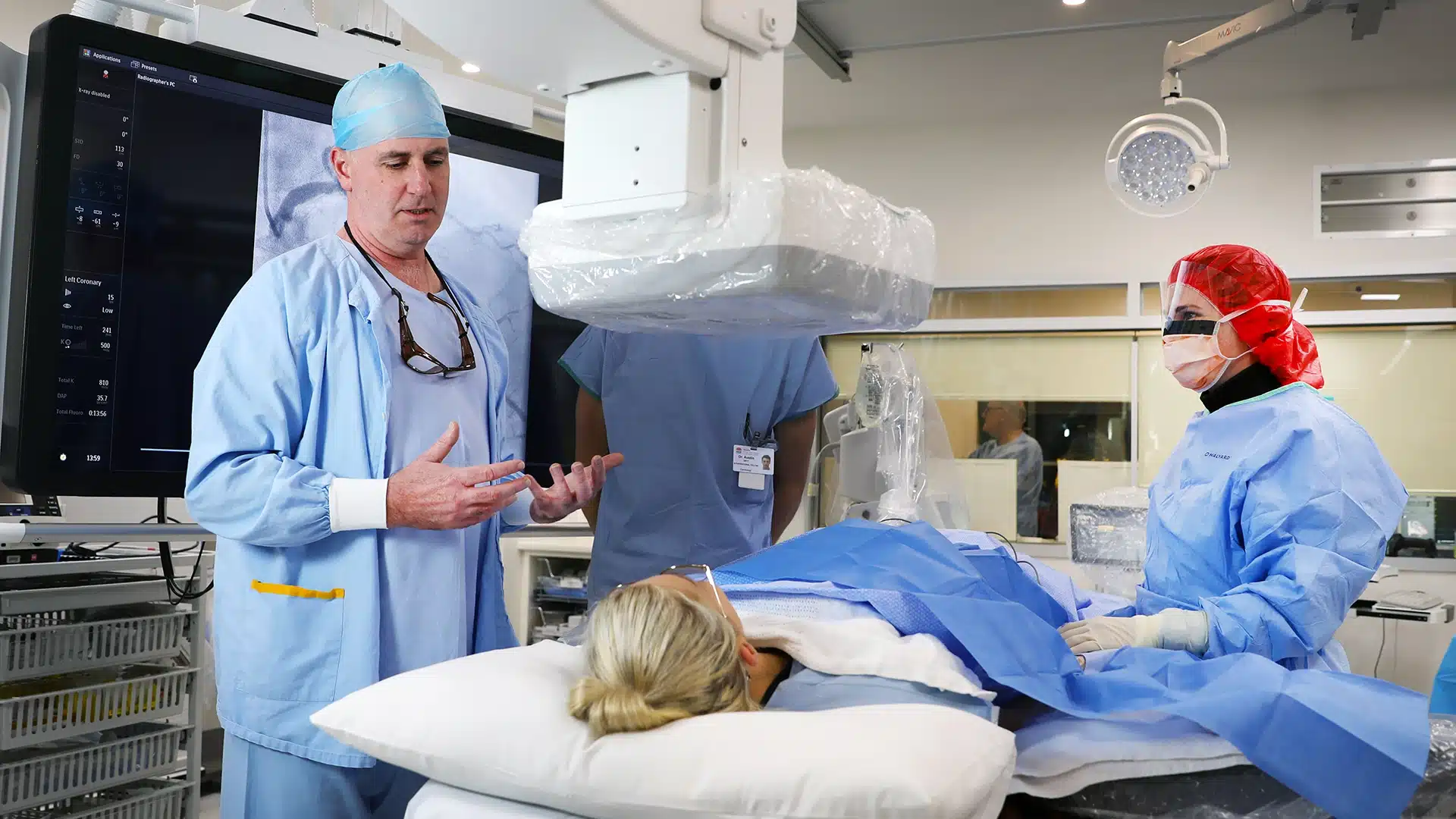





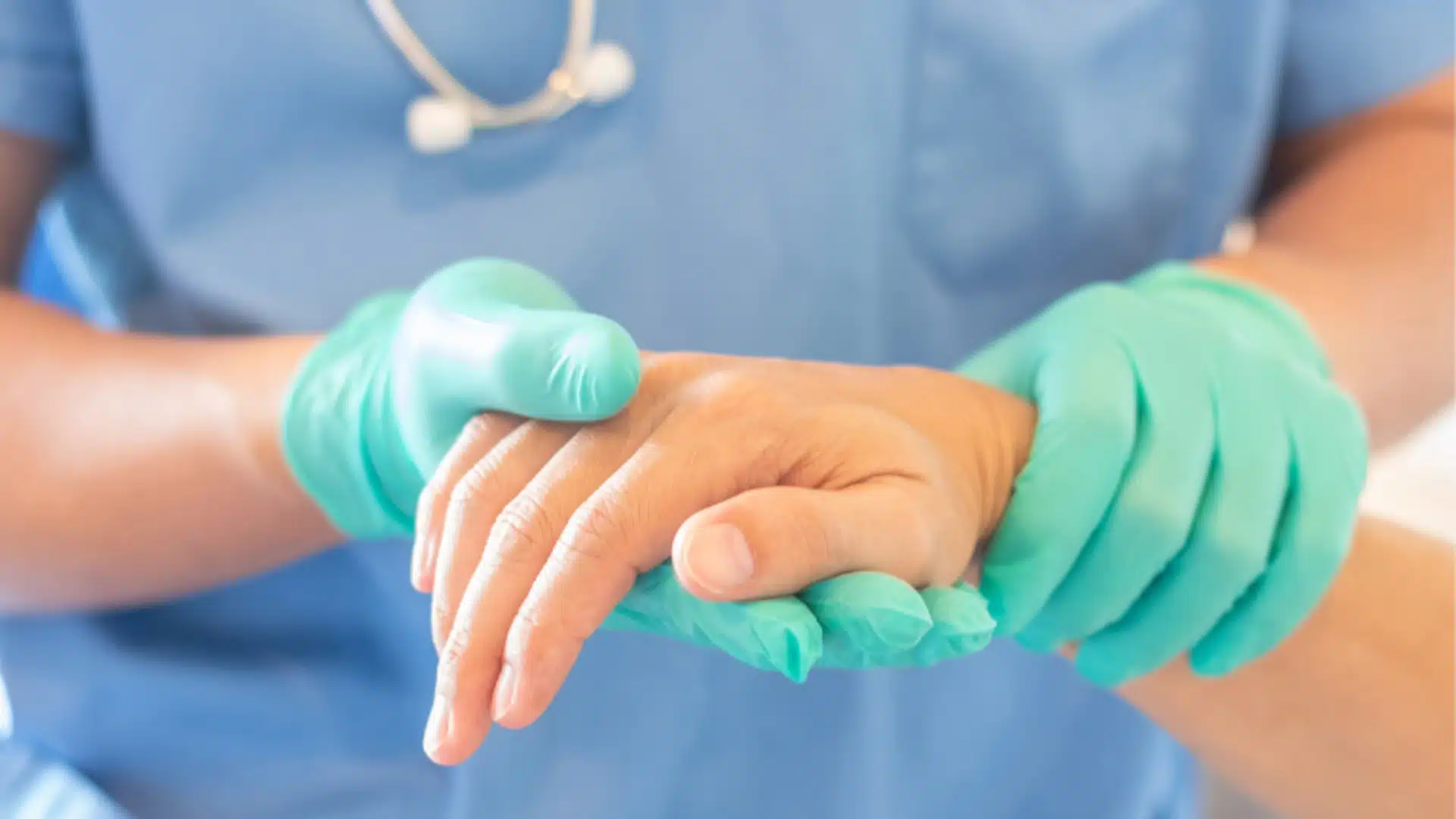

Help us find solutions that prevent illness and allow people to have longer, healthier, happier lives.
Help us find solutions that prevent illness and allow people to have longer, healthier, happier lives.

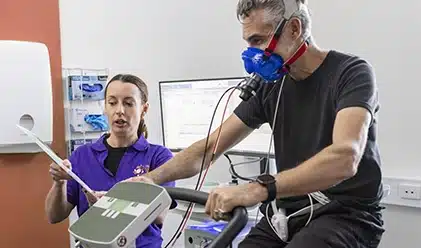
Help our researchers make the next breakthrough. Take part in a real-life research study today.

Partnerships are the key to driving health and medical impact. Invest in our brightest minds and promising discoveries.


Partnerships are the key to driving health and medical impact. Invest in our brightest minds and promising discoveries.

Help our researchers make the next breakthrough. Take part in a real-life research study today.
HMRI would like to acknowledge the Traditional Custodians of the land on which we work and live, the Awabakal and Worimi peoples, and pay our respects to Elders past and present. We recognise and respect their cultural heritage and beliefs and their continued connection to their land.
Hunter Medical Research Institute
We’re taking healthy further.
Locked Bag 1000
New Lambton
NSW, Australia, 2305


This site is protected by reCAPTCHA and the Google Privacy Policy and Terms of Service apply.
Copyright © 2024 Hunter Medical Research Institute | ABN: 27 081 436 919
Site by Marlin Communications
