Emergency department nurses across NSW will gain valuable real-time experience in stroke care thanks to a new virtual reality (VR) training program developed by the Centre for Advanced Training Systems at the University of Newcastle.

Responding to a need for rural, regional and remote areas to have access to regular high-quality training, the TACTICS VR program provides nurses with immersive, interactive and evidence-based training to improve outcomes for people presenting with stroke.
Program director and University of Newcastle Professor Rohan Walker said stroke was a time-critical medical emergency and ensuring fast response and treatment times was essential to saving lives and improving stroke recovery.
“By simulating real-time scenarios, the TACTICS VR training program gives emergency nurses essential practise in how to handle those first critical minutes when a patient presents with stroke,” Professor Walker said.
“This VR training is particularly critical in rural, regional and remote areas where there is a greater chance of less experienced staff treating stroke patients, where they treat fewer stroke cases and have limited access to high-quality training.”
“This is the fourth stroke training module we’ve produced using the TACTICS VR program, and our previous work confirms healthcare staff find the training easy to use and it improves their confidence in best-practice clinical care.”
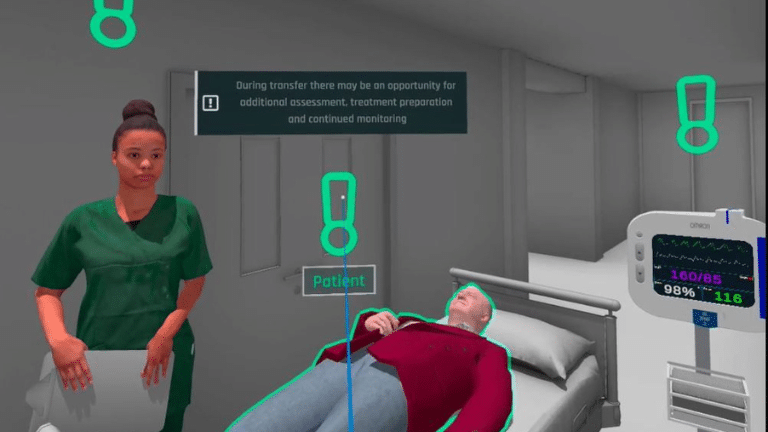
A collaboration between the University of Newcastle’s Centre for Advanced Training Systems, nurses from NSW Health, and the NSW Health’s Agency for Clinical Innovation, the TACTICS VR stroke training program replicates a real-world emergency room inside a VR headset.
TACTICS VR Project lead Dr Steven Maltby said the nurses undertaking the training are required to navigate their role as a stroke patient presents to hospital, and manage their workflow processes through various scenes, including pre-hospital assessment and preparation, initial patient assessment, imaging and monitoring of the patient, and treatment and consent.
Professor Walker said the goal in the development of the training was to put specific emphasis on the nurse’s role in emergency stroke management.
“The aim of the training is to increase awareness of nursing processes in hyper-acute management and emphasise the critical importance of effective communication and team coordination in the first 24-hours after stroke,” Professor Walker said.
So far 25 VR headsets have been distributed to regional and metropolitan hospitals, with a focus on smaller hospitals where staff may have limited exposure to stroke.
NSW Health Deputy Secretary Clinical Innovation and Research and Chief Executive, Agency for Clinical Innovation, Dr Jean-Frédéric Levesque, said the VR training was another innovative way the public health system was using technology to improve patient care.
“VR training gives patients and clinicians access to best-practice stroke care, especially in regional areas where a local hospital does not receive the same volume of stroke patients as its city counterparts,” Dr Levesque said.
“This new training program complements the successful NSW Telestroke Service, which uses video consultation to provide people living in rural and regional NSW with rapid access to specialist stroke diagnoses and treatment. Telestroke is now operating in 23 hospitals across the state.”